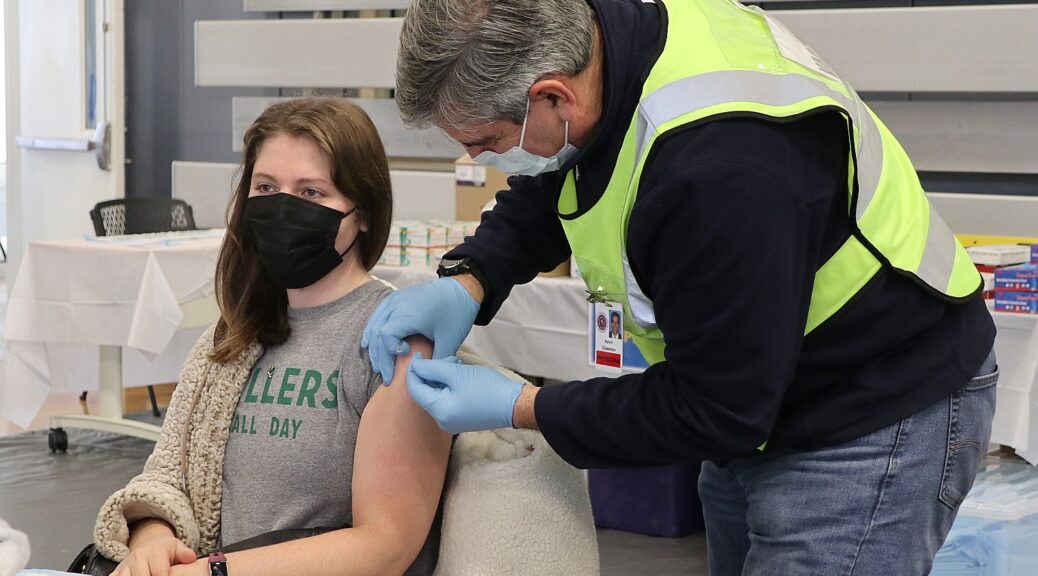
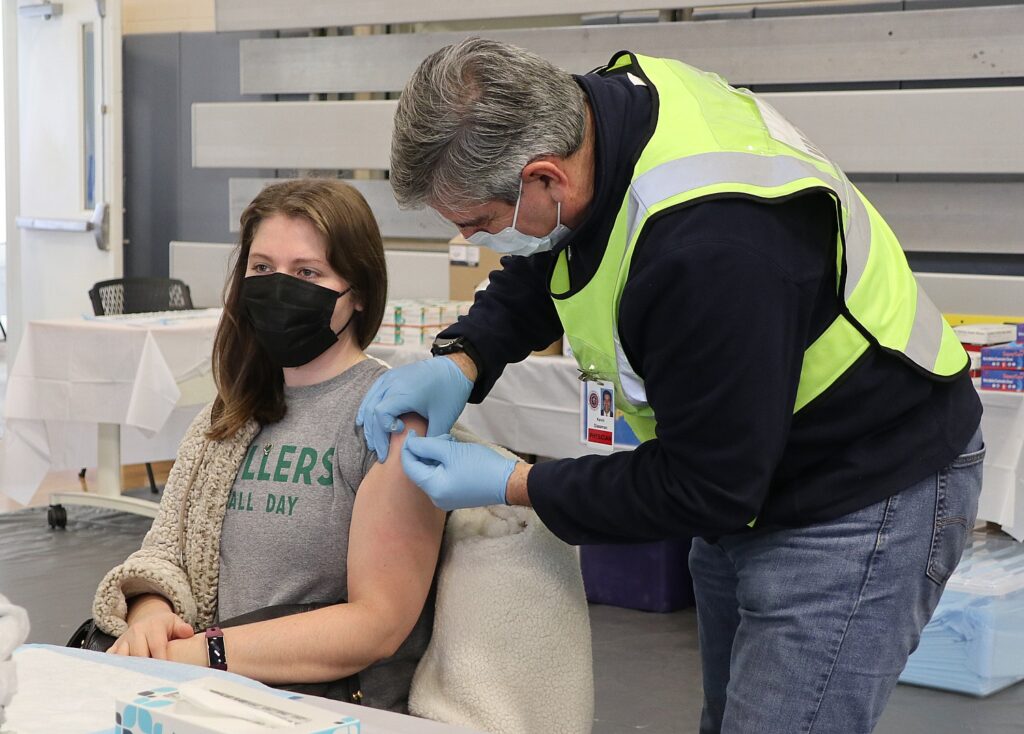
Administration focused efforts on making vaccinations, testin, and treatments even more widely available and accessible as COVID-19 cases increase
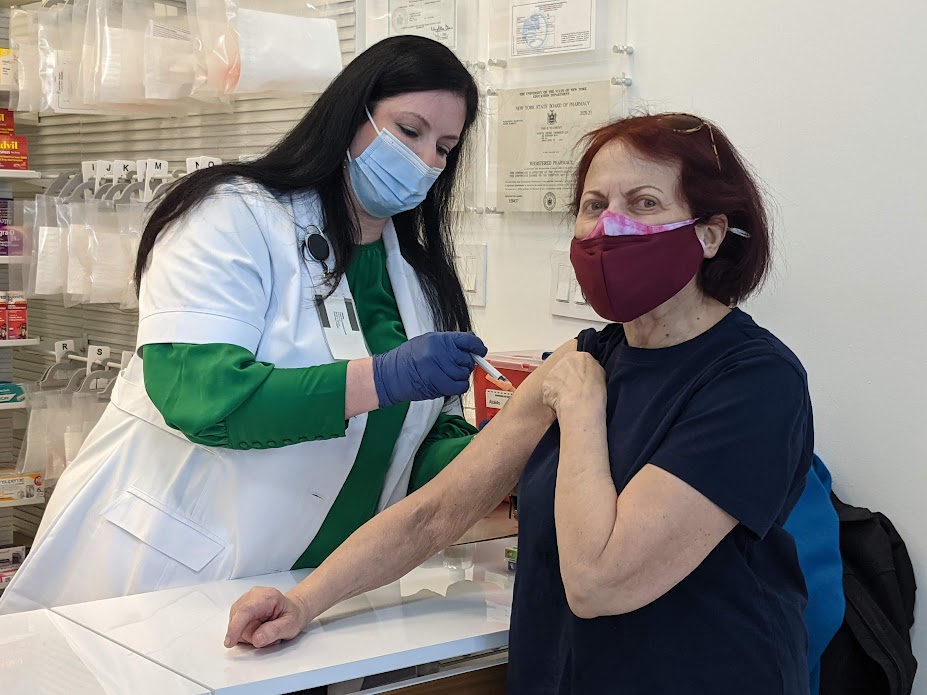
The Biden Administration announced a plan to stay ahead of an increase in COVID-19 cases this winter. While COVID-19 is not the disruptive force it once was, the virus continues to evolve, and cases are on the rise again as families are spending more time indoors and gathering for the holidays. Throughout the COVID-19 response, this Administration has been prepared for whatever the virus throws our way – and this moment is no different.
The Administration’s COVID-19 Winter Preparedness Plan includes:
Expanding easy access to free COVID-19 testing options in the winter. COVID-19 testing is an important tool to help mitigate and slow the spread of the virus. The Administration is encouraging Americans to use at-home COVID-19 tests when they have symptoms of COVID-19, before and after traveling for the holidays, or visiting indoors with immunocompromised or vulnerable individuals. The Administration has made free COVID-19 testing widely available and easily accessible. This includes providing over 15,000 free community testing sites nationwide, covering over-the-counter tests under Medicare, and requiring all health insurance plans to cover eight free at-home tests per month per individual, which can be easily accessed at local pharmacies and online. Ahead of continued increases in cases, the Administration is taking new action to ensure that all Americans have easy and free access to COVID-19 tests in the winter months.
- Making free at-home, rapid COVID-19 tests available through COVIDTests.gov. The Administration is announcing that COVIDTests.gov is open for a limited round of ordering this winter. Starting today, all U.S. households can order a total of four at-home COVID-19 tests that will be mailed directly to them for free. In the absence of Congress providing additional funding for the nation’s COVID-19 response, the Administration has acted with its limited existing funding to add more at-home COVID-19 tests to the nation’s stockpile and support this round of ordering ahead of continued increases in COVID-19 cases. Orders for this round of testing will begin to ship starting the week of December 19th and continue in the weeks ahead. The Administration will also make tests available to individuals who are blind or have low-vision through this program. People who have difficulty accessing the internet or need additional support placing an order can call 1-800-232-0233 (TTY 1-888-720-7489) to get help in English, Spanish, and more than 150 other languages – 8:00 a.m. to midnight E.T., seven days a week. For more information, people can visit www.COVIDTests.gov.
- Distributing more free tests to Americans at trusted locations. In addition to continuing to support access to free COVID-19 tests in schools, community health centers, rural health clinics, long-term care facilities, and other convenient locations, the Administration is announcing additional distribution programs to reach people with free, at-home tests. This includes distributing free at-home tests at more than 6,500 Department of Housing and Urban Development-assisted rental housing properties serving seniors; and expanding a program to distribute free at-home tests to as many as 500 major food banks for them to distribute to people in their communities.
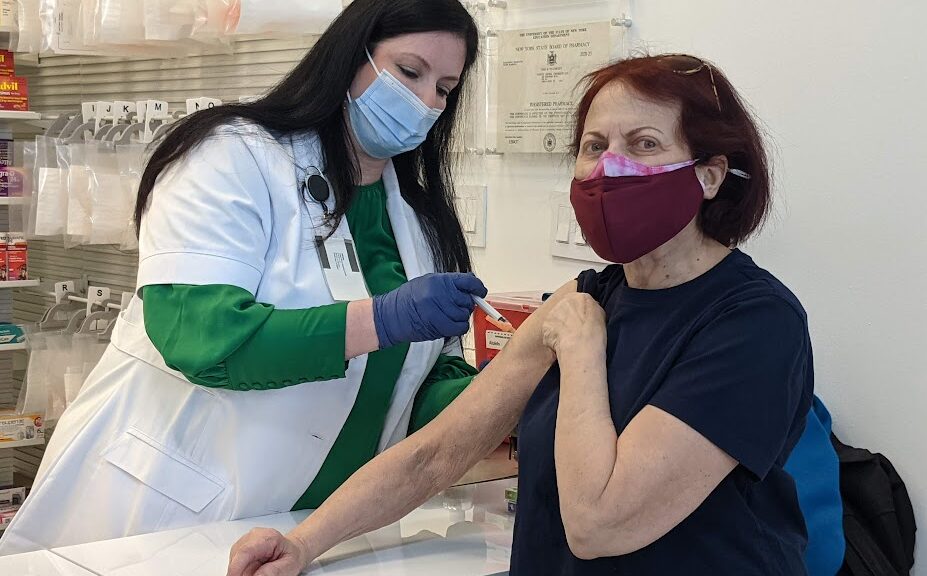
Making vaccinations and treatments readily available to all Americans as cases rise. As we have throughout the pandemic, the federal government continues to leverage all capabilities to support state, local, territorial, and Tribal communities to prepare for, prevent, and respond to increased incidence of COVID-19. That includes working with states, medical providers, businesses, and other groups to expand awareness about updated COVID-19 vaccines, highly effective treatments, and resources to stand up additional vaccination sites and other delivery options to make it easier and more convenient to get vaccinations and treatments.
- Offering resources and assistance to increase vaccinations and respond to a possible surge. Today, U.S. Health and Human Services Secretary Xavier Becerra is sending a letter to all governors outlining key actions that he would like state leaders to take as they prepare for increased cases and hospitalizations this winter, and reminding them of federal supports that are available for their COVID-19 responses. This includes setting up additional mobile and pop-up vaccination sites, surge testing sites, as well as Test to Treat sites where Americans can not only get tested for free, but also can get prescribed and dispensed safe, effective COVID-19 treatments right on site if they test positive and treatment is appropriate for them.
- Collaborating with communities to open pop-up and/or mobile vaccination sites. Communities across the nation are answering the call to expand vaccine access through the increased presence of mobile and pop-up vaccination clinics. This includes efforts in Los Angeles County to open up to 800 pop-up clinics per week; expanded use of mobile vaccination, testing, and treatment units, as well as outbound vaccine and treatment calls to people age 65 and older, at-home administration of vaccines and free home delivery of treatments in New York City; and an increase in Chicago’s at-home vaccine administration program, which provides vaccines for up to 10 people per visit in their place of residence. The Administration has been engaging jurisdictions on the availability of federal resources to continue and increase these efforts, including through use of flexible single-dose vials, and will continue to engage state, local, Tribal, and territorial leaders in the weeks ahead.
- Getting additional resources to community health centers and aging and disability networks to support COVID-19 vaccination efforts. The Administration for Community Living is awarding $125 million to support community-based organizations in the aging and disability networks to hold accessible vaccine clinics and provide in-home vaccinations, transportation, and other supportive services to increase COVID-19 vaccinations for older adults and people with disabilities.
Preparing personnel and resources. Together with states, we will monitor the impacts of variants, cases, and hospitalizations on our communities and – should it become necessary – escalate our support to states and communities. The Administration stands ready with federal capabilities to support urgent needs as they present, including through clinical staffing, personal protective equipment and supplies, and technical assistance.
Readying clinical personnel for deployment as needed to support jurisdictions. The Administration continues to make federal teams and medical personnel available to alleviate strains on hospitals and health care systems through the Department of Health and Human Services’ (HHS’) Administration for Strategic Preparedness and Response (ASPR), the U.S. Public Health Services Corps, and the Department of Defense. Federal agencies can also help offer support for states to take actions, such as providing more flexibility to hospitals balancing patients and staffing, exercising telemedicine options, pursuing staffing options such as contracts, and employing the National Guard to help alleviate strains on health and medical facilities.
- Pre-positioning critical supplies from the Strategic National Stockpile. Tanks to the President’s leadership, the U.S. government has hundreds of millions of N-95 masks, billions of gloves, tens of millions of gowns, and over 100,000 ventilators stored in the Strategic National Stockpile—all ready to ship out if and when states need them. The Administration has pre-positioned these supplies in strategic locations across the country so that we can send them to states that need them immediately.
- Closely monitoring emerging variants and assessing their potential impacts on testing, treatments and vaccines. This winter, federal agencies will continue to monitor Omicron subvariants and the spread of any other emerging variants of the virus in the United States. This includes genomic surveillance of specimens from representative populations to detect new variants and to monitor trends in currently circulating variants. The Centers for Disease Control and Prevention (CDC) tracks and reports on genomic sequencing results from a variety of sources, including public health and commercial laboratories. CDC also recently expanded variant reporting from additional sources, including wastewater and through international air travel. The Traveler-Based Genomic Surveillance Program currently collects samples from international air travelers arriving from more than 25 countries at several major U.S. airports. This data, which provides an early warning system for detection of variants and trends over time, is publicly shared on the CDC COVID-19 Data Tracker.
Focusing on protecting the highest-risk Americans. As we have done since the beginning of the Administration, we remain focused on meeting the needs and protecting Americans at highest risk of severe illness from COVID-19. This includes residents of nursing homes and other congregate care facilities, where we know vaccination rates remain too low. This also includes older Americans, individuals who are immunocompromised, disabled individuals, and others who face a higher risk of severe illness and death from COVID-19.
- Releasing a winter playbook for nursing homes and long-term care facilities. The Administration will release a winter playbook for administrators of nursing homes and long-term care facilities that summarizes the actions these facilities should take to reduce serious illness, prevent hospitalizations and deaths, and minimize disruptions in their communities. Nursing homes often serve residents at great risk of severe illness and death from COVID-19, and congregate care settings have an increased risk of spread of respiratory infections. All facilities should take concrete actions to ensure that every resident is educated on and offered an updated COVID-19 shot; that every resident who tests positive for COVID-19 is evaluated and offered treatment; and that every facility is taking steps to improve its indoor air quality.
- Expanding the pool of providers that may administer COVID-19 vaccinations. In addition to working with their partners, staff at nursing homes will now be able to administer COVID-19 vaccines to all residents. HHS will work with states to launch teams and use partner with their Quality Improvement Organizations (QIOs), home health agencies, and Emergency Medical Technicians to deliver vaccines to residents of long-term care facilities. On December 1, 2022, the Centers for Medicare & Medicaid Services (CMS) also added COVID-19 vaccination rates of health care staff and the residents at these facilities to the “Measures under Consideration” list, the list of measures it will potentially consider for certain Medicare quality payment programs, reinforcing its commitment to increased vaccination and improving outcomes for patients.
- Reaching out to governors on nursing home vaccinations. In Secretary Becerra’s letter to governors reminding them of available federal COVID-19 supports, he also highlighted how their states are performing as compared to their peers on vaccinating residents of long-term care facilities, and asked governors for their assistance and partnership in increasing COVID-19 vaccination rates for long-term care residents and staff. CMS leadership will also be reaching out to the jurisdictions with the lowest vaccination rates at these long-term care facilities to remind them of what additional steps they can take to increase vaccination rates among seniors and long-term care facility residents.
- Encouraging hospitals to offer COVID-19 vaccinations to patients before discharge. HHS leadership, including Secretary Becerra, has called upon hospitals through direct outreach to vaccinate their unvaccinated patients or make sure they are up-to-date on COVID-19 vaccinations before they are discharged, especially if they are heading to a nursing home.
- Expanding access to high-quality masks in communities. In January 2022, HHS made up to 400 million N-95 respirators from the Strategic National Stockpile available through tens of thousands of locations including pharmacies and grocery stores, so Americans could have convenient, free access to high-quality masks. About 270 million masks were sent out as part of this initiative, with many still available in stores nationwide. To expand access to these high-quality masks, HHS will offer guidance to participating pharmacies and grocery stores on how they can to work with local health clinics, aging and disability networks, community-based organizations, and health departments to distribute these masks more widely, so that any spare inventory can be utilized through distribution to even more locations.
- Ensuring that every individual has a plan for COVID-19 this winter. With updated COVID-19 vaccines, at-home tests, and effective oral antiviral treatments widely available, the Administration encourages every individual American to have a plan for how to prevent and respond to COVID-19 this winter. CDC has launched a COVID-19 Personal Action Plan, an easy-to-use guide for individuals, caregivers, and clinicians that helps guide individuals through making a plan for where to access free tests, the location of their closest Test to Treat site, and what to ask their provider on treatments if they test positive. The Personal Action Plan helps lay these steps out in an easy-to-use template so that all Americans – especially those at highest risk for severe illness – can decrease the risk of COVID-19 and, if they become infected, have a plan to quickly seek out treatment and avoid its worst outcomes.