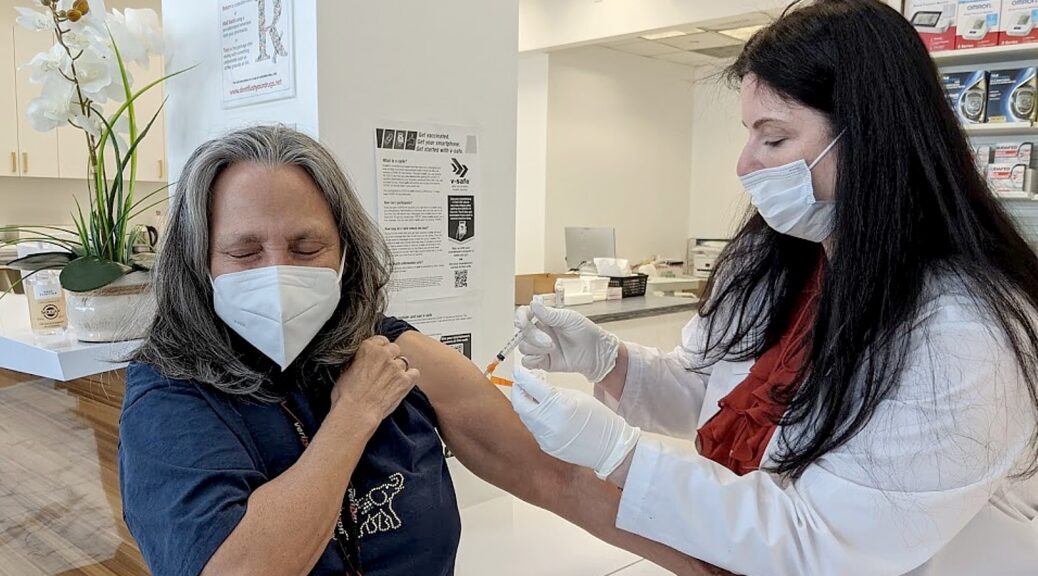
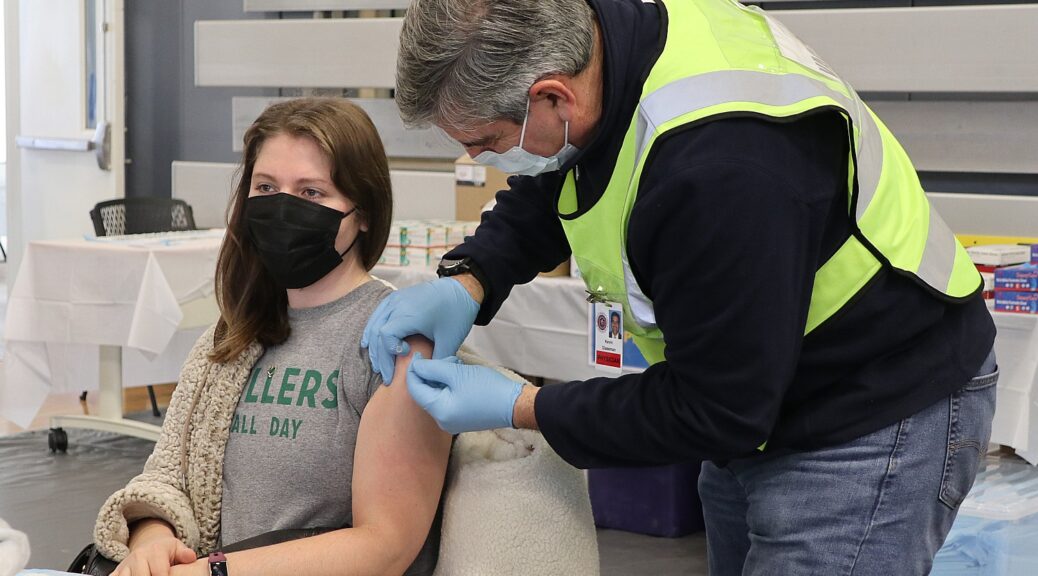
Statewide Indoor Business Mask or Vaccine Requirement to be Lifted Starting February 10, Remains Optional for Businesses, Local Governments, Counties
Masks Will Still Be Required In Hospitals, Nursing Homes, Shelters, Transportation and Other Related Entities
Requirements Related To Masks in Schools Continue and Will Be Reevaluated in Early March, After Mid-Winter Break, Based on Public Health Data
Health Care, Business and Labor Leaders Praise Governor Hochul’s Scientific, Evidence-Based COVID-19 Response
Governor Kathy Hochul today announced New York’s new Winter Toolkit for the new phase of the pandemic, aiming to keep New York safe, open and moving forward. The Winter Toolkit focuses on five core areas: protecting the most vulnerable New Yorkers, increasing vaccinations and boosters, strengthening our health care system, empowering local leaders, and supporting individuals facing the long-term effects of COVID.
“As we begin a new phase in our response to this pandemic, my top priority is making sure we keep New York safe, open and moving forward,” Governor Hochul said. “I want to thank the health care workers, business owners and everyday New Yorkers who acted responsibly during the Omicron surge by masking up and getting vaccinated. But make no mistake: while we’re moving in the right direction, this pandemic isn’t over and our new Winter Toolkit shows us the path forward.”
Governor Hochul announced that the statewide indoor business mask-or-vaccine requirement will be lifted starting Thursday, February, 10, and will remain optional for businesses, local governments and counties to enforce. This protocol, a temporary measure implemented on December 10 as statewide cases spiked, was an effective tool to address the winter surge and the rise of the Omicron variant. With case counts plummeting and hospitalizations sharply declining, this temporary measure is no longer needed statewide. Counties, cities, and businesses will be able to opt into the mask-or-vaccine requirement if they so choose.
Masks remain a critical tool to fight the spread of COVID-19, and mask requirements will remain in place in certain high-density settings. All health care settings regulated by the Department of Health and other related state agencies will continue to require masks. Masks will also be required in nursing homes, adult care facilities, correctional facilities, detention centers, homeless shelters, and domestic violence shelters, public transit and transportation hubs, as well as trains, planes and airports in accordance with federal regulations.
Governor Hochul also announced plans to assess the mask requirement in schools in early March, to ensure students can continue learning in-person and in the classroom. The assessment will be based on public health data, including key metrics like cases per 100,000 residents, hospital admission rates, vaccination rates, global trends and pediatric hospitalizations. Plans are already underway to distribute two tests for every K-12 student ahead of midwinter break, and continue distribution the following week when students return to school. In the meantime, Governor Hochul has directed the Department of Health to work on preliminary guidance, with input from educators and parents, to keep students and teachers safe.
With a new phase of the pandemic beginning, Governor Hochul unveiled a new Winter Toolkit to help keep New Yorkers safe. The toolkit includes efforts to:
- Protect the most vulnerable
- Increase access to vaccines, boosters and testing
- Strengthen the health system
- Empower local leaders
- Support New Yorkers facing long-term COVID effects
Protecting the Most Vulnerable
New York State will continue to acquire and distribute masks and tests to New Yorkers to ensure those who need them can access them. The state’s test stockpile contains 92 million tests. Over 14.2 million tests have been distributed to schools and tests will continue to be distributed as needed. 4.2 tests have been distributed to nursing homes, 2.4 million tests to adult care/congregate facilities, and 4 million tests to counties.
1.28 million masks have been distributed to nursing homes and 5.5 million masks have been distributed to counties.
Visitation rules in nursing homes will remain in place. Visitors must show proof of a negative test within 24 hours of their visit and masks will remain required.
Tests will be made widely available for students so that K-12 student can go home for their Midwinter Break with two tests.
Increase Access to Vaccines, Boosters and Testing
- New York State’s mass vaccination and testing sites will remain open to ensure all eligible New Yorkers can access first, second, and third doses for themselves and their children.
- The State’s #VaxForKids pop-up programming continues to expand with 63 new sites established today and 193 sites established to date. This effort brings the vaccine directly to parents, guardians, and their children at local schools, community centers, and destinations like farmer’s markets to make getting vaccinated convenient and accessible for families.
- New York State is actively preparing for the Pfizer-BioNTech vaccine to come online for children under 5 years old.
- The State’s robust education efforts to reach New Yorkers with good, science-based information about the vaccine is on-going including through traditional advertising, digital and multimedia campaigns, and direct messaging efforts through SMS text messaging, robo-calling, and Excelsior Pass push notifications.
- All 61 state-operated and state-partnered testing sites will remain open to provide New Yorkers with access to COVID-19 testing.
- Testing also remains widely available at over 1,800 sites statewide in every region of the State.
Strengthen the Healthcare System
To troubleshoot shortage issues, Executive Order 4 to increase staffing flexibility will remain in place. National Guard will continue to be trained to be able to staff in places needed as well.
As part of the Governor’s Winter Surge Plan 2.0, the State has already deployed 20-member Medical Specialty Teams from the U.S. military hospital support team to Erie County Medical Center, a 35-member team to SUNY Upstate in Syracuse, 92 new ambulance teams to different regions in the state, including 50 to NYC, and two Medical Specialty Teams (MSTs) of 20 personnel from the Department of Defense to Strong Memorial Hospital.
Governor Hochul also outlined investments to strengthen the health care system in her 2022 State of the State Address and FY 2023 Budget. $10 billion will be invested to grow the health care workforce by twenty percent in five years. $4 billion will be invested in wages and bonuses to stop the hemorrhaging of health care staff. $1.6 billion will be invested via the Capital Plan.
Empower Local Leaders
Governor Hochul’s announcement today comes after consultation with local leaders on steps the state is taking to fight COVID-19.
Support New Yorkers Facing Long-Term COVID Effects
- Last Thursday, the State’s Department of Health hosted an expert forum on Long COVID and over 2,000 individuals registered to view the panels. Panelists included specialists, clinicians, social scientists, patients and advocates who shared their experience, expertise, and insights.
- This discussion, as well as continued focus and study by the Department, will inform the State’s response which will span policy, regulatory, and program considerations to support New Yorkers suffering from long COVID as well as the healthcare providers who care for them.
State Health Commissioner Dr. Mary T. Bassett said:”At every stage of the pandemic, and since Omicron emerged, the Department of Health has monitored the science to inform the State’s data-driven COVID-19 response. Today, we have reached a critical point in our fight in which the proof of vaccination or masking requirement for businesses, restaurants and other indoor public spaces will expire. As the winter surge recedes, getting vaccinated and boosted remains critical to continue the progress we’ve made, and masking remains key to keeping children in schools safely and keeping everyone safe in public transit and other crowded settings. As we continue to assess the data, the Department is also focused on ensuring the necessary support is there for those suffering from long COVID.”
President & CEO of Northwell Health Mike Dowling said,”I support the Governor’s decision. It is reasonable and data driven. It is now time to begin the pivot to a more normal way of living”.
Business Council of New York State President & CEO Heather Briccetti said,“As protecting public health remains our top concern, we also appreciate the Governor’s efforts to assure that state policies reflect ever-changing COVID levels. Throughout the pandemic, employers have taken the necessary safety precautions and followed state and federal guidelines to ensure the safety of their employees and customers. We hope new policies will encourage New Yorkers to continue to support New York businesses still recovering from the pandemic.”
New York State Association of Counties President Martha Sauerbrey said, “We applaud Governor Kathy Hochul’s decision to lift the statewide mask mandate and allow for local decision-making regarding COVID-19 prevention measures. Local leaders and health officials have the training and public health expertise to ensure the health and safety of the public at large. Any step toward normalcy is a good step for our residents and businesses who have struggled so hard to protect one another for nearly two years. We acknowledge Governor Hochul’s public health measures, including testing, vaccinations and emergency management assistance, during this pandemic and appreciate the steps she took to address this wave without implementing other business restrictions. Now we welcome the opportunity to return communicable disease control to the counties.”
Partnership for New York City President & CEO Kathryn Wylde said, “Governor Hochul’s decision to allow expiration of mask mandates in the workplace will encourage the return of employees to the office and accelerate the city’s economic recovery. It is the right call.”
“The mask mandate has helped keep New York’s working men and women safe and healthy during the most uncertain and volatile moments of the public health crisis,” Building and Construction Trades Council of Greater New York President Gary LaBarbera said.”The easing of indoor mask mandates for businesses is a positive sign in New York’s recovery, as it’s a direct result of COVID-19 cases dropping across the state and, hopefully, the pandemic itself receding. We’re grateful to Governor Hochul for her thoughtful and steady leadership in navigating New York through these uncertain times.”
New York State AFL-CIO President Mario Cilento said, “In light of the announcement today, we thank the governor for ensuring employers still have responsibilities under state statute, including the Public Employee Safety and Health Act and the New York HERO Act, which remain in effect. These laws establish safety protocols to protect workers and the public. Moving forward, in the absence of the mask mandate, employers must continue to work with their employees to make sure appropriate protections are in place.”
New York State Restaurant Association President & CEO Melissa Fleischut said, “As protecting public health remains our top concern, we also appreciate the Governor’s efforts to assure that state policies reflect ever-changing COVID levels. Throughout the pandemic, employers have taken the necessary safety precautions and followed state and federal guidelines to ensure the safety of their employees and customers. We hope new policies will encourage New Yorkers to continue to support New York businesses still recovering from the pandemic.”
Retail Council of New York State President & CEO Melissa O’Connor said, “Governor Hochul over the past several weeks has prioritized the health and safety of New Yorkers, while recognizing the importance of keeping the economy open during the COVID-19 ‘winter surge’ in New York. Today’s announcement is a positive development for retailers throughout the state and we will continue to collaborate with the Governor on economic recovery efforts.”
Greater New York Hospital Association President Kenneth Raske said, The Greater New York Hospital Association fully supports Governor Hochul’s decision to let the mask mandates expire. Thankfully, hospitalizations due to COVID have dropped dramatically in recent weeks and we are optimistic that this trend will continue, particularly as more and more New Yorkers get vaccinated. Returning to as much normalcy as possible is exactly what is needed. We thank the Governor for her outstanding leadership during this extraordinarily challenging time and, as always, stand ready to assist in any way needed to combat this pandemic. Erie County Medical Center President & CEO Thomas J. Quatroche Jr., PhD said, “Governor Hochul clearly understood that the restaurant industry could not survive another shutdown, and the mask mandate helped ensure that we could remain open for indoor dining even as cases surged. Now as the metrics continue to trend in the right direction and consumer confidence increases, we remain hopeful that better times are ahead and we can continue our recovery from the darkest days of the pandemic. This measur